Pregnancy is a precious journey filled with joy, curiosity, and responsibilities. Among the many health decisions you make, one of the most important is taking the right vaccines during pregnancy. These vaccinations offer protection not only to the mother but also to the unborn child.
Why Vaccines Matter in Pregnancy
During pregnancy, a woman’s immune system changes, making her more vulnerable to certain infections. Vaccines help boost immunity and create antibodies. These antibodies pass through the placenta, helping to protect the baby in its early months of life.
Dr. Shelly Singh, a well-known gynecologist, strongly advises pregnant women to stay updated on their vaccinations. According to her, “Prevention is always better than cure, especially when it involves two lives.”
Key Vaccines Every Pregnant Woman Should Know About Vaccines during pregnancy
Let’s look at the main vaccines recommended during pregnancy.
1. Td Vaccine
The Td vaccine offers protection against tetanus and diphtheria. It is often given early in the pregnancy and is considered safe for both mother and baby.
This vaccine replaced the older TT vaccine due to an increase in diphtheria cases. Getting the Td vaccine is usually part of standard prenatal care in India.
2. Tdap Vaccine
The Tdap vaccine in pregnancy protects against tetanus, diphtheria, and pertussis (commonly known as whooping cough). Whooping cough can be deadly for infants, especially in the first few months of life when they are not fully immunized.
Health experts recommend taking the Tdap vaccine between 27 to 36 weeks of pregnancy. This is the ideal time for the mother’s body to create and transfer antibodies to the baby.
Dr. Shelly Singh emphasizes the importance of this vaccine in each pregnancy, even if the mother has taken it before. She also advises family members and caregivers to take the vaccine as part of the “cocooning” strategy, which helps shield the newborn.
3. Influenza Vaccine
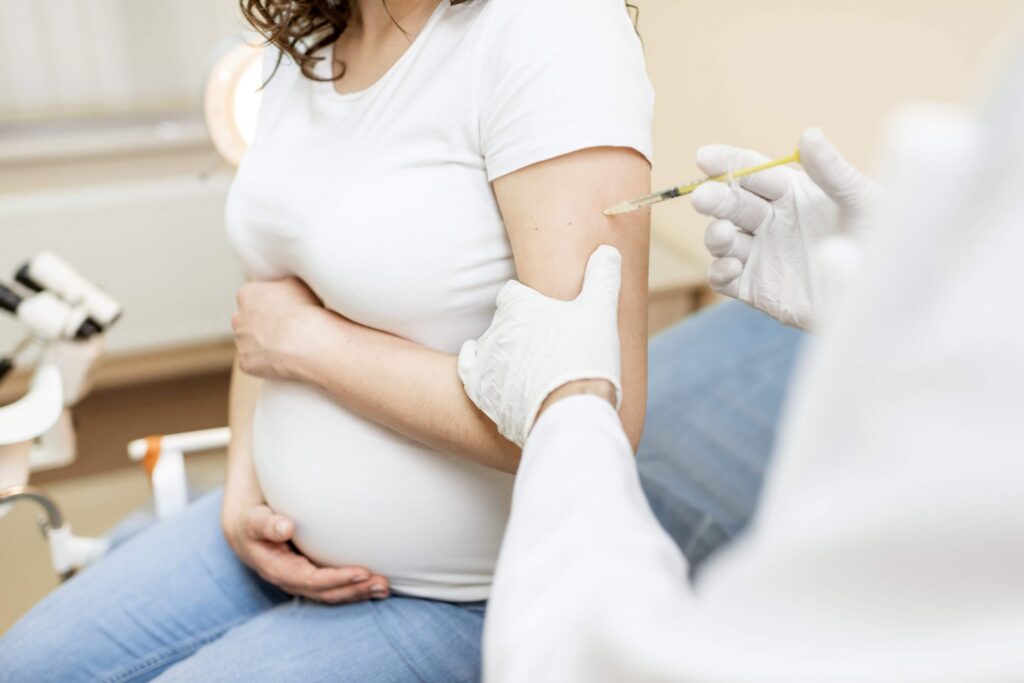
The influenza Vaccines during pregnancy protects the mother from seasonal flu, which can become severe and even life-threatening. Pregnant women are more likely to develop complications from the flu compared to other adults.
This vaccine can be taken at any point during pregnancy, but ideally before the flu season begins. Getting vaccinated also helps protect the baby in the first few months of life.
Dr. Shelly Singh says, “Pregnant women who catch the flu often experience more serious symptoms. The flu shot can prevent this and also protect the baby after birth.”
4. Hepatitis B Vaccine
The Hepatitis B Vaccines during pregnancy is given only to women who are at higher risk. This includes healthcare workers, individuals with Hepatitis B-positive partners, and those who have a history of multiple sexual partners or drug use.
If a woman has already started the Hepatitis B vaccine series before becoming pregnant, she can safely continue it during pregnancy under her doctor’s guidance.
Are These Vaccines Safe?
Yes, all recommended Vaccines during pregnancy are considered safe. Most of them do not contain live viruses and are well-tolerated.
Side effects, if any, are usually mild and short-lived. These may include a slight fever or soreness at the injection site. However, the benefits far outweigh the risks.
Dr. Shelly Singh assures her patients that these vaccines go through strict safety checks and are regularly recommended by health authorities like WHO and ICMR.
When to Get Vaccinated?
- Tdap: Between 27 and 36 weeks
- Td: First trimester or early second trimester
- Influenza: Before or during flu season
- Hepatitis B: As advised, based on risk level
Final Thoughts
Taking Vaccines during pregnancy is a vital step in protecting both mother and baby from preventable diseases. It also reduces the chances of complications during and after delivery.
Don’t wait for symptoms to appear—vaccination is all about prevention. It’s a simple yet powerful way to give your baby a healthy start in life.
Dr. Shelly Singh, with her years of experience, always encourages her patients to make informed choices about pregnancy care, including immunization.
Book Your Appointment Today
If you’re expecting or planning to conceive, consult with Dr. Shelly Singh to discuss your vaccination schedule. With her expert guidance, you can enjoy a safer and healthier pregnancy.
Call now or book online to schedule your consultation with Dr. Shelly Singh. Your journey to motherhood deserves the best protection.

















